
BARIATRIC SURGERY
Gastric Balloon
Gastric balloon in Istanbul — non-surgical, temporary intragastric balloon for BMI 27–35. Placed endoscopically, worn for 6 or 12 months, removed. Paired with nutrition coaching to build lasting habits. Medical oversight Dr. Güleş, JCI-accredited hospitals. From €1,850.
from €2,150 All-inclusive
Trusted by 10,000+ international patients
JCIAccredited Hospitals
T.C.Ministry of Health Licensed
ISAPSBoard-Certified Surgeons
4.9 ★Trustpilot · 1,200+ reviews
15+ yrsYears of Experience
8,000+Procedures Performed
Get Your Free Consultation
Our medical team will review your case and send you a personalized treatment plan within 24 hours.
Global Price Comparison
Save up to 82% in Istanbul
Typical all-inclusive prices by country. Sources: ASPS, RealSelf, major UK/US clinic rate sheets, 2025.
🇹🇷
Turkey (Istanbul)
from €2,150
save 82%
🇬🇧
United Kingdom
from €9,500
🇺🇸
United States
from €12,000
🇮🇹
Italy
from €6,500
🇩🇪
Germany
from €6,500
Duration
20–30 minutes
Anesthesia
Sedation
Hospital Stay
Day procedure
Back to Work
3 days
Recovery Time
3–5 days
Results Visible
6–12 months
Gastric balloon is a non-surgical, temporary weight-management tool. A soft silicone balloon is placed endoscopically in the stomach, filled with saline, and left in place for six or twelve months (depending on the device chosen). It occupies stomach space, slows gastric emptying, and reduces meal capacity — producing weight loss of typically 10–20% of body weight over the treatment period. At the end of the period, the balloon is removed endoscopically.
We describe it at the start as a tool, not a solution — because that is the honest framing, and it is what determines whether a given patient will benefit or regret. The balloon works during the months it is in place. What happens afterwards is determined by what behaviour has changed. For patients who treat the six or twelve months as a window to rebuild their relationship with food and develop sustainable habits, the balloon is a useful intervention. For patients who treat it as a quick fix and return to pre-balloon eating patterns on removal, weight regain over the following year is common.
Who gastric balloon is suitable for
The right candidate typically has BMI in the 27–35 range — above overweight, below the threshold where sleeve or bypass become indicated; has tried non-surgical weight loss (diet, exercise, and often GLP-1 medication) with limited success, and wants a structural aid to make the next attempt successful; is willing to engage with a structured nutrition and behaviour-change programme during the treatment period (this is the non-negotiable piece); does not have active gastrointestinal conditions that contraindicate endoscopic placement (large hiatus hernia, peptic ulcer disease, previous gastric surgery, active H. pylori infection — these are screened before placement).
Who should not have a balloon: patients with BMI over 35 and comorbidities (sleeve or bypass is the correct operation, not balloon); patients with BMI under 27 (the medical indication is not present); patients with active GORD/reflux disease (balloon can worsen it); pregnant patients or those planning pregnancy in the next year.
Balloon or GLP-1 — which is right?
This is the question most anglosphere patients arrive with, because GLP-1 medications (Ozempic, Wegovy, Mounjaro) are now widely available in the UK, US, Australia and elsewhere. Both produce weight loss; both are temporary (weight regain on stopping is common); both work better paired with behaviour change.
Balloon is typically the better choice when: you want a one-time intervention over 6–12 months rather than an ongoing medication; cost makes ongoing GLP-1 medication (~£200+/month privately) unsustainable long-term; you have experienced GLP-1 side effects (nausea, GI discomfort, hair thinning) that you want to avoid; or you have tried GLP-1 and regained after stopping, and want a different tool for the next attempt.
GLP-1 is typically the better choice when: you prefer a medical over a procedural intervention; you want the option of continuing long-term; you have specific medical indications beyond weight loss (type 2 diabetes, cardiovascular risk); balloon placement is contraindicated.
At consultation we discuss both honestly. For a subset of patients, the right answer is GLP-1, not balloon — and we say so.
The balloon types
Two main device categories are used. The choice depends on the patient and the treatment window.
Fluid-filled endoscopic balloon (6 or 12 months): placed endoscopically under light sedation, filled with saline and methylene blue (the dye turns urine blue if the balloon leaks, providing an early warning). Worn 6 or 12 months. Removed endoscopically. The workhorse device and our typical recommendation.
Swallowable balloon (Allurion — 4 months): swallowed as a capsule, expands in the stomach, and passes naturally through the GI tract at approximately month four without removal. Less weight-loss time and lower overall weight loss, but no placement or removal procedure. Indicated for specific patients who want the shortest-window option.
The procedure, step by step
Placement is performed endoscopically under light intravenous sedation. The procedure takes 20–30 minutes. No surgical incisions. Day-procedure — you return to the hotel after a brief recovery period. In a JCI-accredited hospital.
Removal (at 6 or 12 months depending on device) is also endoscopic, under light sedation, typically 15–20 minutes. Performed at our partner clinic if you are able to return to Istanbul, or — for patients unable to travel back — arranged at a recommended clinic in your home country. We coordinate both options at the time of initial placement.
Recovery and the first weeks
The first three to seven days after placement are the most difficult. The stomach is adjusting to the balloon — nausea, mild-to-moderate abdominal discomfort and reduced appetite are expected and are treated with anti-emetic and anti-spasmodic medications provided at discharge. Most patients take this period significantly — rest, hydration, and very gradual reintroduction of food according to the provided protocol.
By the end of week one, most patients are eating normally (but significantly less) and returning to normal activity. Weight loss typically begins during this initial adjustment period and continues throughout the treatment window.
The nutrition and behaviour-change programme — non-negotiable
Balloon without behaviour change produces temporary weight loss and near-certain regain. For that reason, every balloon we place includes a 12-month nutrition and behaviour-change programme (even for 6-month balloons — we continue support for 6 months after removal). The programme includes English-speaking nutritionist support via WhatsApp for meal planning and troubleshooting, monthly check-ins on weight and behaviour patterns, and specific behavioural focus areas depending on your profile (emotional eating, portion control, alcohol, meal timing, exercise integration).
Patients who engage with the programme consistently achieve the best and most durable outcomes. Patients who do not engage typically regain weight within 12–18 months of removal. We are honest about this at consultation.
Expected outcomes
Typical weight loss during treatment: 10–20% of body weight over the treatment window, with substantial individual variation. Weight at 12 months post-removal: for patients engaged with the behaviour programme, most sustain the large majority of loss; for patients who disengage, significant regain is common.
Risks and realistic expectations
Honest risks: nausea and abdominal discomfort in the first week (expected, well-treated); intolerance requiring early removal in a small percentage of patients; balloon deflation (rare — detected by blue urine from methylene blue dye); early migration (very rare with current devices); reflux/GORD; risks of endoscopic placement and sedation (minimal in a JCI-accredited setting with an anaesthesiologist).
The most relevant "risk" is regain post-removal if behaviour hasn't changed. We frame this explicitly as the primary determinant of long-term outcome.
Why Istanbul versus other destinations
Endoscopic experience volume matters for both placement safety and for the quality of the supporting programme. Our team places balloons regularly, in JCI-accredited hospitals with an anaesthesiologist present, with an integrated English-speaking nutrition team for the 12-month pathway. The price gap versus UK/US/Australia is substantial.
**Dr. Mustafa Ekrem Güleş** approves every patient clinically before placement.
Why not the €800 gastric balloon
On balloon, the rock-bottom price is paid in non-JCI settings, no nutrition programme (the balloon becomes a temporary weight-loss tool with no long-term benefit), and no pathway if you experience intolerance or need early removal. A clinic quoting balloon at €800 often excludes the nutrition programme, excludes anaesthesia costs, excludes removal, and has no follow-up staff in English.
What you pay for with us is verifiable: JCI-accredited hospital with anaesthesiologist, placement and removal (both included), 12-month English-speaking nutrition programme, pathway for early-removal if required.
English-speaking team — for the full 12-month journey
Our team replies in English on WhatsApp, phone and email. For balloon patients specifically, the 12-month programme includes an English-speaking nutritionist available throughout for meal planning, symptom troubleshooting and behaviour coaching. The balloon period is a focused 12 months of change — we support it in English from start to finish.
Request your free consultation — our team replies in UK/IE business hours and in a second window covering US Eastern through Australian morning. BMI-based candidacy assessment and an honest balloon-vs-GLP-1 recommendation on the same day.
What's Included
VIP airport transfer (pickup & drop-off)
Accommodation in 4-star partner hotel
Professional translator with 24/7 support
All hospital and surgery fees
Pre-operative blood tests & medical consultation
Anesthesia (general or local as required)
Post-operative medications & aftercare kit
1-year follow-up consultations
Dedicated WhatsApp patient coordinator (24/7)
Not Included
International flights to and from Istanbul
Additional hotel nights beyond the package
Personal expenses (minibar, spa, shopping)
Frequently Asked Questions
What is a gastric balloon?
A gastric balloon is a soft silicone balloon inserted into your stomach via endoscopy (no surgery). It takes up space, reducing appetite and portion sizes. It's typically left in place for 6 months, then removed.
How much weight can I lose with a gastric balloon?
Most patients lose 15–25 lbs (7–11 kg) over 6 months with a gastric balloon. It's less dramatic than surgery but helpful for those wanting to test whether they can commit to lifestyle changes before permanent surgery.
How much does a gastric balloon cost?
Gastric balloon insertion at Estetica costs €2,200–€2,800, including placement, removal, and all follow-up visits. This is one of the most affordable weight-loss interventions and often covered partially by medical tourism packages.
Is balloon insertion painful?
No. The procedure is done under mild sedation via endoscopy. You'll feel pressure but no pain. Most patients wake up with mild bloating and nausea for 2–3 days, managed with anti-nausea medication.
What can I eat with a balloon?
You'll start with liquids and soft foods for the first week. Then normal foods in smaller portions. The balloon takes up ~50% of stomach space, so full feelings arrive quickly. Protein, vegetables, and hydration are priorities.
Can I remove the balloon early if I'm uncomfortable?
Yes. If you experience severe nausea, vomiting, or other complications, the balloon can be removed early via endoscopy. However, most discomfort resolves within the first 3–5 days as your stomach adapts.
Deep Dive
All articles →Further Reading
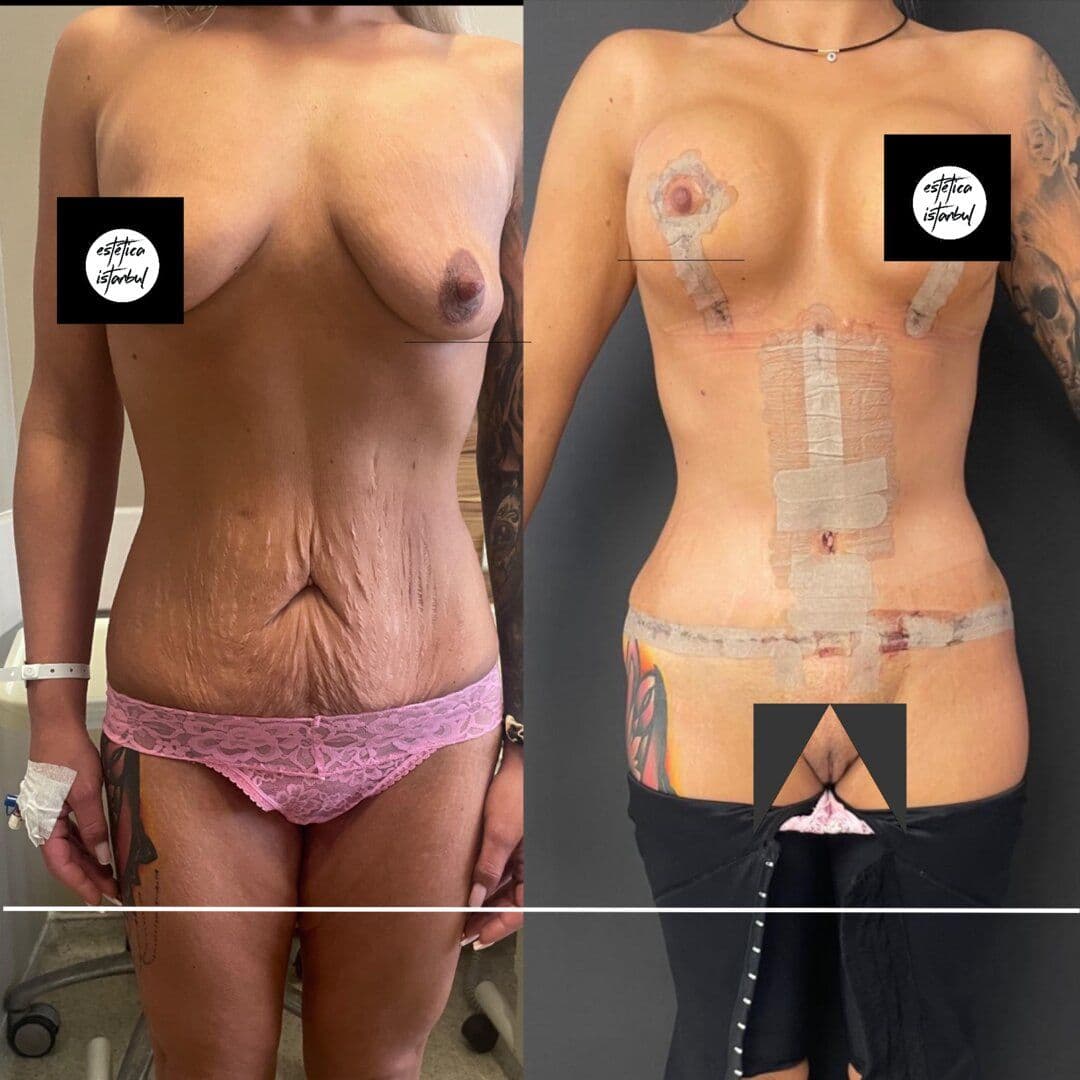
Medical Tourism
Plastic Surgery Tips to Have a Slimmer Body
Each of us is uniquely beautiful and our body type is a reflection of that. Sometimes, however, we may want to make changes to our bodies to feel better and increase our self-confidence. This is where plastic surgery offers effective options to...
Medical Tourism
Botched Facelift: What You Need to Know
Today, as the interest in aesthetic interventions increases, sometimes undesirable results may occur. Especially in facelift procedures, the practices of inexperienced or unqualified professionals can cause bad results. So, how can...

Medical Tourism
What Is JCI Certification and Why It Matters for Medical Tourism
Discover what JCI certification means, how to verify it, and why choosing an accredited clinic is essential for your medical tourism safety and success.